
MIPS: Quality Category – Let’s Take a Look
December 12, 2016
Written by Sarah Leake
For the 2017 reporting year, the MIPS Quality Category will account for 60% of the overall MIPS performance score. The Quality category replaces PQRS that eligible clinicians may already be familiar with.
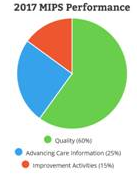
Most participants will report 6 quality measures, including one outcome measure, for at least 90 days in order be eligible for a possible positive adjustment. For groups reporting via the CMS web interface, you must report 15 quality measures for a full year.
There are 271 total measures available to choose from in 2017, down from 283 in 2016. Seventy-one of those measures are outcome measures. A tool is available for searching and filtering the 271 measures to find what is best for you. Click here to see this tool. There is an alternative to download the complete list of 271 measures in a CSV file for more robust analysis.

A key change with the MIPS Quality Category is no longer the option of using measure groups for reporting individual clinicians. However, you can select measures based on your specialty, please see below for the list of specialty measure sets. If you find that your specialty measure set does not have an outcome measure listed, you are allowed to substitute the outcome measure for a high priority measure that fits your specialty better.

Resource Links
Leave a reply, ask a question or share information using the “Leave a Reply” section below, or email Sarah Leake directly with your questions or comments.
Read all previous posts
See PQRS Blog
Subscribe to the Merit-Based Incentive Payment System (MIPS) Blog
Subscribe
See a list of upcoming webinars
Check out any webinars you missed

Leave a Reply